Twilight’s Edward and Bella – Romance or Rabies? A scientific view on vampires
Today, September 28th, is world rabies day! Rabies is an animal borne viral disease that kills nearly 100 percent of its victims once the infection reaches the brain. But have you ever wondered how this fatal virus can affect the brain, causing victims to become ´rabid´? I was thinking about it in those autumn days when all these pumpkin-spice lattes and fancy Hokkaido soups around the city indicate that Halloween is just around the corner – which is always a good excuse to enjoy classic splatter movies like Shawn of the Dead or the zombie film I Am Legend once again, or get on line to be the first to see the latest Twilight movie this November.
I am not the only scientist wondering where all this interest might come from. In 1998 the Spanish physician Juan Gòmez-Alonso proposed in the top-tier journal Neurology that scary tales of vampires and werewolves, mythologized in Hollywood movies and TV shows, may have a factual basis – originating from stories of humans infected with the rabies virus.
The parallels are quite interesting:
Both rabies and vampirism are transmitted by a bite. Both cause face spasms, hydrophobia (a fear of water) and an inability to face one’s own reflection in a mirror. Both show a hypersexualized behavior, with male rabies patients ejaculating up to 30 times per day in the final stages of infection. Finally, contrary to the Hollywood interpretation of a vampire living for centuries, the earliest mythology put the life span of a vampire at about 40 days, similar to the time is takes untreated rabies to kill a human. Gòmez-Alonso also found more evidence when examining geography and culture: geographic areas that experienced particularly devastating epidemic rabies outbreaks in the past – like the Balkans – are rich in popular folkloric myths and legends about vampires and hematofages (animals feeding on blood) with different features and behaviors.
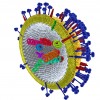
The rabies is a virus belonging to the Rhabdoviridae family. It is a highly fatal disease that causes acute encephalitis, responsible for approximately 55,000 deaths each year worldwide, mainly in Asia and Africa. In 2010, the United States reported 6,153 animal cases of rabies across all states (including Puerto Rico) with the exception of Hawaii. Luckily, human acquisition of rabies in the US is a relatively rare occurrence, with only 2 human cases recorded for the same year (CDC data).However, the yearly mortality rate in other countries is significantly higher; for example, in India more than 25,000 people fall victim to rabies each year.
The rabies virus reproduces in both humans and animals, and is found in not only nervous tissue, but also in saliva, making the transmission of the virus easier….a bite will do. Non-animal associated transmission of rabies is extremely rare, but has occurred by means of transplant surgery.
The normal mode of transmission of this disease is by direct contact between animal and man. The animal implicated most frequently is man’s best friend – the dog, causing 99% of human rabies deaths – but other common zoonotic reservoirs (zoonosis meaning that an infectious disease can be transmitted between species) of the disease include bats, foxes, and skunks. Transmission from bats occurs through direct bites, skin-to-skin contact and through inhalation of aerosolized bat feces (like in caves with high bat populations).
The primary wild reservoir of rabies in the US is Procyon lotor, or the common raccoon; and the highest density of raccoons in New York State is…. New York City! The rabies population is under tight observation by the city health department because New York City experienced a Rabies Outbreak in 2009–2010 in New York´s favorite dog-walking destinations Central Park and Inwood Hill Park. It took one year of trapping and vaccinating animals before the numbers significantly dropped back to 1 reported case in 2012.
The rabies virus reproduces in both human and animal reservoirs, and is found in not only nervous tissue, but also in saliva, making the transmission of the virus easier….a bite will do. Transmission from bats occurs through direct bites, skin-to-skin contact and through inhalation of aerosolized bat feces (like in caves with high bat populations).
Non-animal associated transmission of rabies is extremely rare.
After a typical human infection by a dog bite, rabies replicates in muscles and spreads from the bite wound into the peripheral nervous system, moving about 1–2cm per day. It then travels along the nerves from the peripheral nervous system to the central nervous system (CNS), driven by an unknown mechanism. The period between the inoculation of the virus into the victim/host and its invasion of the CNS is the incubation period. The median incubation period is 85 days (range 40–150 days). During this phase, the virus causes quite diffuse and nonspecific symptoms within the host, including fever, sore throat, chills, malaise, anorexia, headache, nausea, vomiting, shortness of breath, cough, and weakness.
At this stage vaccination can still initiate cell-mediated immunity to prevent symptomatic rabies. But once the virus reaches the brain treatment is useless; it quickly causes encephalitis and more extreme symptoms appear. This is called the “prodromal” phase and patients die within weeks.
There are two forms of canine rabies in the prodromal phase, a “furious” (encephalitic) or “dumb” (paralytic) form. Furious rabies is characterized by high fever, hyperactivity, hypersexuality, including an increase in sexual appetite and priapism (a painful medical condition, in which the erect penis or clitoris does not return to its flaccid state) of several days, along with dysfunction of the autonomic nervous system, and abnormal looking pupils (WHO). It is this form or rabies that people think of when they hear the word “rabies,” especially as the autonomic dysfunction also includes excess salivation, producing the famous “foaming at the mouth.”
The dumb form progresses from the peripheral weakness around the transmission area to a generalized craniospinal weakness and cumulates in final encephalitis (inflammation of the brain).
On a cellular level rabies can be diagnosed prior to the appearance of symptoms by the presence of Negri bodies (inclusion bodies found in nerve cells) and a direct fluorescent antibody test (dFA). However, the dFA test requires brain tissue, and is therefore performed post-mortem. It is the test of choice for the testing of rabid animals but for living humans it is necessary to perform several other tests to diagnose rabies before death. The two main tests are PCR-based tests on saliva, or testing the blood serum or spinal fluid for antibodies. Additionally, skin biopsy specimens of hair follicles may display a rabies antigen within skin nerves.
So, happy World Rabies Day and have fun at the movies – now you can watch the films as a scientist as well as a horror fan!
———————————————–
Further reading:
Juan Gomez-Alonso; Rabies : A possible explanation for the vampire legend, Neurology 1998;51;856
Rabid: A Cultural History of the World’s Most Diabolical Virus
by Bill Wasik, Monica Murphy, Viking, www.penguin.com
| Print article | This entry was posted by Christine Marizzi on September 28, 2012 at 9:32 am, and is filed under G2C Online. Follow any responses to this post through RSS 2.0. You can leave a response or trackback from your own site. |